Is Lifestyle Medicine a Scam?
Or rather, is lifestyle medicine enough?
I’ve been asking myself this recently.
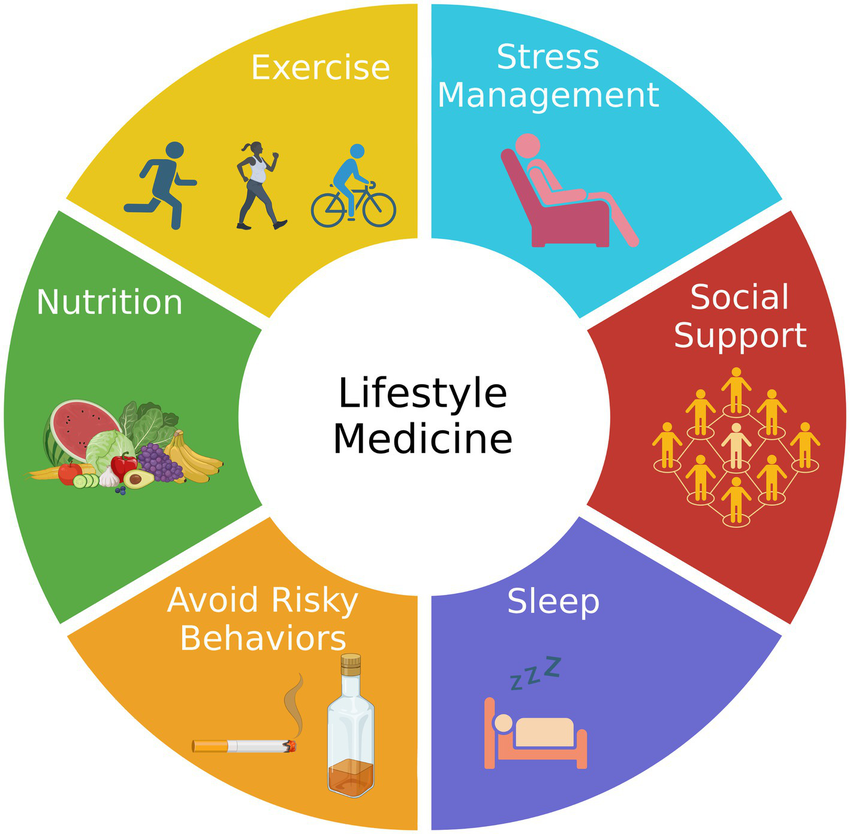
Lifestyle medicine asks individuals to eat better, move more, sleep well, manage stress, avoid harmful substances, and build connections. These pillars are evidence-based and powerful. In my clinic, I see their benefits daily. But when we present lifestyle change as the solution—without naming the conditions that constrain choice-we drift into a quiet moralisation of health.
Lifestyle medicine is necessary, but not sufficient.
When the structural determinants of well-being are not addressed, “choose better” only works if the choice is genuinely available.
A woman working two jobs on unpredictable shifts cannot optimise sleep.
A family living in overcrowded housing cannot “reduce stress.”
A neighbourhood without green space makes “move more” an abstraction.
Ultra-processed foods are cheap, accessible, and aggressively marketed; fresh foods often aren’t.
This is not a failure of motivation. It is a failure of systems.
Decades of public health evidence show that income, education, housing, transport, gender norms, racism, and environmental exposure shape health outcomes as powerfully (often more so)than individual behaviours. The World Health Organisation has been explicit about this for years: where you are born, grow, work, and age predicts your health trajectory long before your willpower enters the room.
There is also a risk we rarely name: when lifestyle medicine is over-emphasised, responsibility quietly shifts from institutions to individuals. Health becomes a personal project rather than a shared societal outcome. Those who cannot comply are labelled “non-adherent,” when in reality they are structurally constrained.
Lifestyle Medicine Omits the Impact of Inequity
As a clinician, I was trained to blame my patients for their 'bad choices'. I wonder if lifestyle medicine is doing the same thing to women?
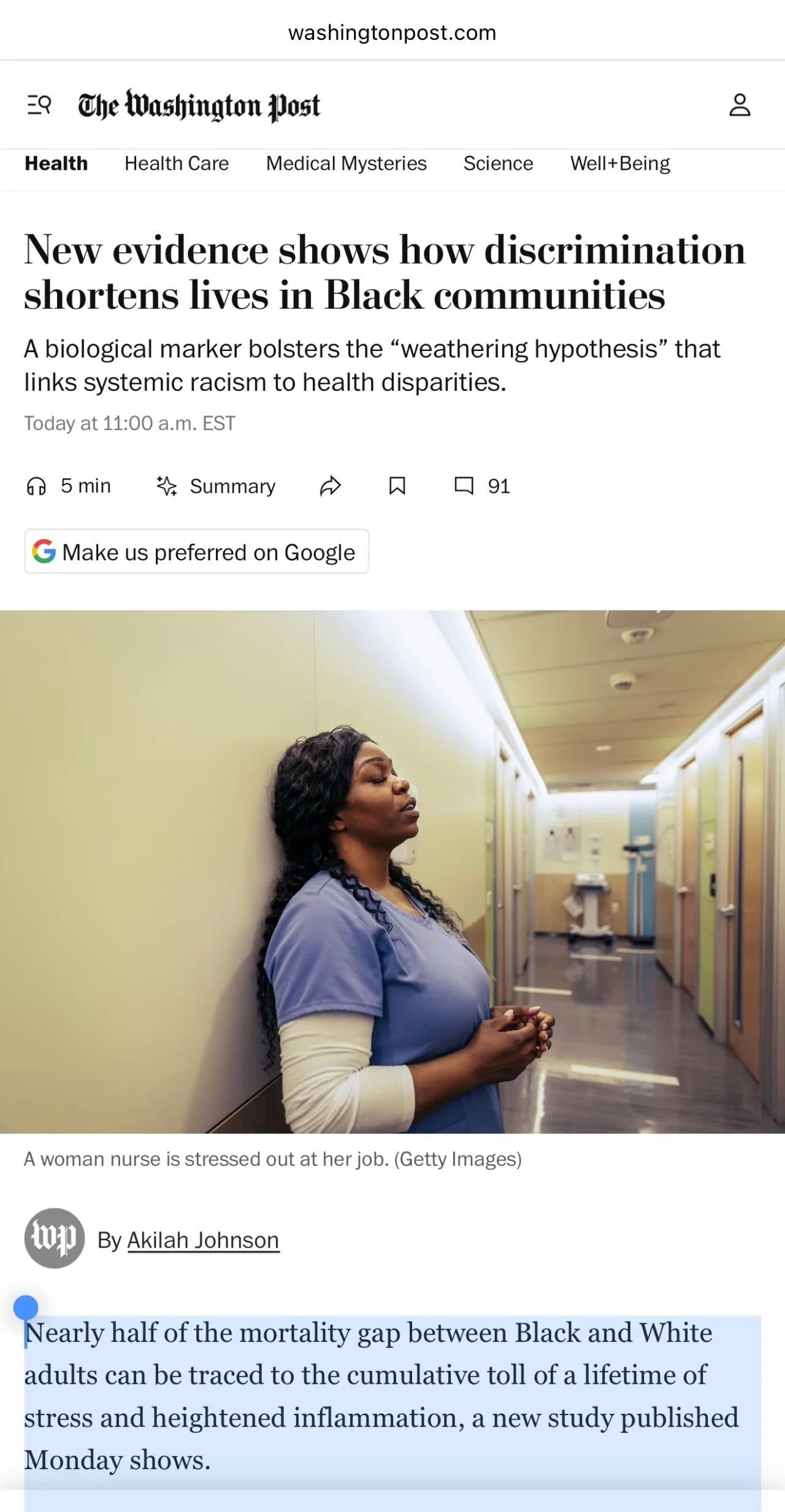
The healthy choice is sometimes harder for women- especially women of colour. New research links discrimination, higher cumulative stress and inflammation to mortality gaps between Black and White individuals.
Lifestyle medicine often arrives wrapped in hope, scented candles, and quiet guilt- layered onto women already expected to parent like they don’t work and work like they don’t parent.
Intersectional disadvantages based on socio-economic status, race & ethnicity, disability and migration compound the inequity gap fostered in lifestyle medicine.
Then the pièce de résistance arrives in the form of perimenopause- brain fog, rage, exhaustion, weight gain, challenged by hormonal shifts- and still the message is: Try harder. Choose better.
So where does that leave lifestyle medicine?
It remains essential-but only when positioned within a broader frame:
As support, not substitution
Lifestyle medicine should complement policy, not replace it. It works best when social protections- living wages, safe housing, parental leave, access to healthcare- are in place to make healthy choices feasible.As a collective, not just individual effort
Behaviour change scales when environments change: walkable cities, affordable nutritious food, clean air, psychologically safe workplaces. Health improves faster when the default is healthy.As trauma-informed and context-aware
Telling people to “manage stress” without acknowledging chronic precarity misses the point. Stress is often a rational response to unstable conditions.As a lever for advocacy
Clinicians and public health professionals can use lifestyle medicine’s evidence base to argue for upstream change (urban planning, labour policy, food systems), not merely downstream counselling.
If we are serious about wellbeing across the life course, across communities, then lifestyle medicine must be paired with structural medicine: policies that redistribute opportunity, reduce exposure to harm, and create conditions in which healthy lives are realistic, not aspirational.
Lifestyle medicine can change lives.
Social determinants decide whose lives are easiest to change. The real question, then, isn’t whether lifestyle medicine is enough.